All published articles of this journal are available on ScienceDirect.
Membranous Nephropathy Associated with Atheroembolism
Abstract
Membranous nephropathy (MN) is one of the most common biopsy diagnoses in adults, and it has been associated with chronic infections, autoimmune diseases, malignancies, and drugs. However, MN associated with cholesterol crystal emboli has never been reported. Here we present a patient with MN as an unusual manifestation of atheroembolism.
A 75-year-old man with worsening renal function after catheter ablation developed moderate proteinuria and underwent a renal biopsy. Findings on light, immunofluorescence, and electron microscopy were all compatible with membranous nephropathy. Moreover, one occluded interlobular artery contained a pathognomonic, biconvex, needle-shaped cleft, which indicated a cholesterol crystal emboli. The degree of proteinuria was in parallel with the number of eosinophils, which indicated a close relationship between MN disease activity and renal atheroembolism. Hypereosinophilic syndrome secondary to atheroembolism may cause MN; thus, corticosteroid therapy was likely to be effective.
INTRODUCTION
Atheroembolization occurs when portions of an atherosclerotic plaque break off and embolize distally, resulting in partial or total occlusion of multiple small arteries including glomerular arterioles, leading to tissue or organ ischemia.
Membranous nephropathy (MN) is the leading cause of nephrotic syndrome in adults. MN is most often primary (idiopathic); however, it has been associated with chronic infections, autoimmune diseases, malignancies, and drugs. Cholesterol crystal embolization to the kidney typically produces a subacute kidney injury; however, MN has never been reported as a renal manifestation of cholesterol crystal emboli.
We describe a case of a patient who presented with blue toe syndrome and livedo reticularis followed by subacute kidney injury after angiography, subsequently developed mild proteinuria and kidney biopsy showed MN concomitant with cholesterol crystal emboli. This case represents an uncommon presentation of atheroemboli.
CASE REPORT
Clinical History and Initial Laboratory Data
A 75-year-old man with a 9-year history of diabetes and hypertension was admitted to nephrology unit of our hospital because of worsening renal function with moderate proteinuria.
The baseline serum creatinine level (SCr) was 1.2 mg/dL, and estimated glomerular filtration rate (eGFR) of 46.0 mL/min/1.73m2, without any proteinuria or active urine sediments. Diabetes had been well controlled under the HbA1c level (percentage National Glycohemoglobin Standardization Program units) of 6.5% with pioglitazone and sitagliptin, and we had not admitted any diabetic retinopathy. After catheter ablation for nonsustained ventricular tachycardia (NSVT) 8 month earlier, he developed discrete gangrenous lesions in the toe (blue toes) and livedo reticularis in the next day, followed by increased SCr to 2.1 mg/dL in 2 weeks. Repeated urinalysis continued to show benign findings with few cells or casts, and neither proteinuria nor hematuria was detected. Clinical and laboratory findings above led him to the diagnosis of an atheroemboism, and he was treated with prednisolone (30 mg/day progressively tapered off). However, his renal function was gradually getting worse to the SCr of 3.65 mg/dL, corresponding to eGFR of 13.6 mL/min/1.73m2, after emergence of proteinuria (1+) with a urinary protein/creatinine ratio (UPCR) of 0.5 g/gCre. Laboratory results are listed in Table 1. To determine the cause of decreased renal function and moderate proteinuria, a kidney biopsy was performed.
| Parameter | Value |
|---|---|
| SCr (mg/dL) | 3.65 |
| SUN (mg/dL) | 27 |
| eGFR (mL/min/1.73m2) | 13.6 |
| Total protein (g/dL) | 5.3 |
| Serum alubumin (g/dL) | 2.8 |
| White blood cell (/μL) | 7400 |
| Eosinophil (/μL) | 1380 |
| Hemoglobin (g/dL) | 10.7 |
| Blood glucose (mg/dL) | 81 |
| Serum calcium (mg/dL) | 5.7 |
| Urinalysis | Protein (1+), blood (-) |
| Urinary protein/creatinine ratio (g/gCre) | 0.5 |
| C3 (mg/dL) | 67 |
| C4 (mg/dL) | 28.3 |
| PR3-ANCA (EU) | 5.7 |
| MPO-ANCA (EU) | <1 |
| ANA | negative |
| IgG (mg/dL) | 1386 |
| IgA (mg/dL) | 452 |
| IgM (mg/dL) | 44 |
| IgE (IU/mL) | 991 |
Kidney Biopsy
The sample submitted for light microscopy contained 26 glomeruli, of which 9 were globally sclerosed. Nonsclerosed glomeruli showed a moderate increase in mesangial matrix with mild proliferative features. Nodular intercapillary gromerulosclerosis (Kimmelstiel–Wilson lesion), which is peculiar to diabetic nephropathy, was not found. There was no evidence of crescent formation, endocapillary proliferation, fibrinoid necrosis or thrombosis. Diffuse thickening of glomerular basement membranes with some spikes was observed with periodic acid–methenamine silver staining. These findings were apparently different from isolated glomerular basement membrane thickening of diabetes mellitus. There was mild interstitial inflammation and interstitial fibrosis. Inflammatory infiltrates consisted of mononuclear cells and plasma cells, but neither eosinophils nor neutrophils were detected. Arteries and arterioles showed mild thickening of the intima particularly in vas afferens, with marked hyaline arteriosclerosis. Moreover, one occluded interlobular artery containing a pathognomonic biconvex, needle-shaped cleft, which indicated a cholesterol crystal. Immunofluorescence microscopy showed granular staining for IgG (2+) and C1q (1+) along glomerular capillary walls, but was negative for IgA, IgM, and C3. IgG4 was also negative in paraffin section, but other subtyping of capillary wall was not obtained. Tubular basement membranes were negative for all staining. Electron microscopy showed focal effacement of podocyte foot processes. Many loops showed small subepithelial electron-dense deposits (EDDs). EDDs were also detected in the mesangium and within the lamina densa, but subendothelial deposits were not present. Representative light, immunofluorescence, immunohistochemistry, and electron microscopy of membranous nephropathy and cholesterol crystal emboli are shown in Fig. (1).
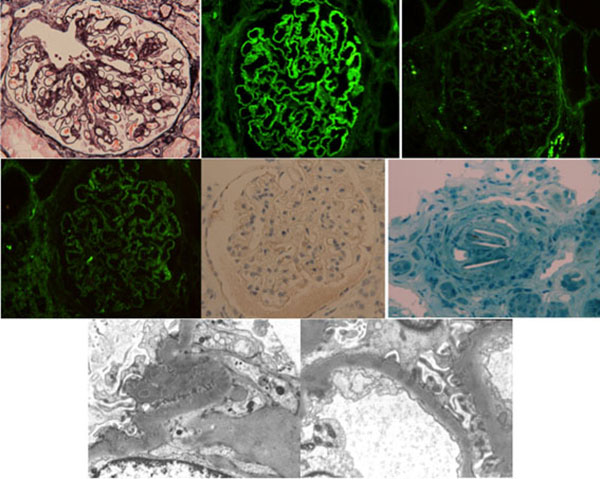
Diagnosis
Kidney needle biopsy: (1) membranous nephropathy and (2) cholesterol crystal emboli.
Clinical Follow-up
Eosinophils were elevated to approximately 1300/μL, with slightly positive PR3-ANCA and decreased C3. Viral antigens, including that of hepatitis B, other autoantibodies suggesting connective tissue diseases, and tumor markers indicating the presence of malignancy, were all negative. Computed tomographic scanning, upper endoscopy, and colonoscopy were also performed to rule out diseases including malignancies that could cause secondary MN; however, they were not detected. Although the patient was followed up as an outpatient with conservative treatments, the SCr level was stable around 3.0 mg/dL and eGFR was 17 mL/min/1.73m2. However 3 months later, the SCr increased to 3.87 mg/dL with eGFR of 12.7 mL/min/1.73m2, accompanied by proteinuria (2+) with UPCR of 1.7 g/gCre (Fig. 2). Marked elevation of eosinophils (5150/μL) was also admitted. Workup for circulating anti-phospholipase A2 receptor (anti-PLA2R) antibodies was negative in the patient’s serum. Prednisolone was re-started and showed marked reduction in UPCR and eosinophil, but eGFR remained stable afterward.

DISCUSSION
Atheroembolization is usually induced by iatrogenic events such as angiography or cardiovascular surgery [1]. Renal involvement is present in 25 to 50 percent of cases, typically with a subacute kidney injury observed within a few weeks or more than several weeks after a possible inciting event [2], often associated with peripheral eosinophilia [3]. Other features include hypocomlementemia, which has been reported in 39% of patients in one study [4]. The urinalysis in patients with renal atheroemboli is typically benign with few cells or casts reflecting renal ischemia, while prominent proteinuria or active urinary sediments including hematuria are rarely admitted [4].
On the other hand, MN is the leading cause of nephrotic syndrome in adults, accounting for over one-third of biopsy diagnoses within primary glomerulonephritis [5]. MN is most often primary, although it has been associated with hepatitis B antigenemia, autoimmune diseases, malignancies, and the use of certain drugs such as gold, penicillamine, anti-TNF-alpha therapy, and nonsteroidal anti-inflammatory drugs [6].
Our patient presented with blue toe syndrome and livedo reticularis in the next day of cardiac ablation for NSVT, followed by weekly decreasing eGFR and accompanied mild proteinuria 6 months later. There was no doubt on the diagnosis of an atheroembolism from clinical course; however, newly admitted proteinuria suggested the coexistence of other glomerular disease. Kidney biopsy showed diffuse thickening of glomerular basement membranes with some spikes, granular staining for IgG on immunofluorescence microscopy, and focal effacement of podocyte foot processes with many loops showing small subepithelial EDDs on electron microscopy: these findings were all compatible to MN. Moreover, a pathognomonic biconvex, needle-shaped cleft was admitted in one occluded interlobular artery, which indicated the existence of renal atheroembolism as a background.
There are several reasons to support the idea that the proteinuria was caused by MN secondary to atheroembolism. First, diabetic nephropathy or focal glomerulosclerosis causing proteinuria was not found in the kidney biopsy. Prominent proteinuria can be described with diabetic nephropathy or focal glomerulosclerosis, which often underlie atheroembolism [7]. However in this case, these findings were not found in the kidney biopsy and no proteinuria had been admitted before the episode. Diabetic retinopathy had not been admitted, either. These support the idea that the proteinuria was caused by superimposed MN. Underlying MN before the episode was also less likely because of the absence of proteinuria at that time. Second, marked elevation of proteinuria associated with increased eosinophils, seen in acute phase of atheroembolism, indicated that MN disease activity of MN and the renal atheroembolism were closely related to each other. Third, in terms of pathological findings, although EDDs are likely to be exclusively subepithelial and intramembranous in idiopathic MN [6], deposits were also detected in the mesangium in this case. Negative IgG4 in parafiin section also decrease the likelihood of primary MN. Furthermore, workup for circulating anti-PLA2R antibodies was negative, which suggested that the MN was not primary. PLA2R is a transmembrane receptor that is highly expressed in granular podocytes, which has been identified as a major antigen with the proportion of approximately 70% in human idiopathic MN [8, 9]. On the contrary, there was no evidence of antibodies in serum from patients with secondary MN, proteinuric conditions other than MN, or from healthy controls. Tissue staining for PLA2R may be more sensitive than circulating anti-PLA2R autoantibodies in primary MN [8], although we could not perform the test. As for secondary MN, no signs of chronic infections, including hepatitis B, autoimmune diseases, and malignancies, were detected. The drugs causing secondary MN were not used either. However, none of the above findings were definite, and the mechanisms of the causal relationship between atheroemboli and MN are unclear. One possible explanation is that marked proteinuria was associated with eosinophilia secondary to the atheroembolism. As shown in our case, eosinophilia and hypocomplementemia frequently occur during the acute phase of an atheroembolism, thereby showing immunological activation at the surface of the exposed emboli [10]. Approximately 20% of idiopathic hypereosinophilic syndrome (HES) patients develop proteinuria and hypertension, and renal manifestations include eosinophilic nephritis, MN, crescentic glomerulonephritis and immunotactoid nephritis, with or without immune deposits [11]. In both previous cases of MN associated with idiopathic HES, proteinuria, and eosinophilia greatly improved with corticosteroid treatment, as in our case in which the degree of proteinuria was closely associated with the eosinophil count [12, 13]
The mechanisms underlying renal involvement of HES were not well described, but were thought to be the same as those implicated in tissue damage of other organs: activated eosinophils release a number of cytopathic substances especially eosinophil granule major basic protein 1, eosinophil peroxidase, and other mediators [14]. Cytotoxicity of these substances can induce tissue damage including renal involvement.
In conclusion, this is the first report of a case to show the possibility of a link between corticosteroid-sensitive MN and atheroembolism. HES secondary to atheroembolism may cause MN, and this type of MN is thought to respond well to corticosteroid treatment.
CONFLICT OF INTEREST
The Authors confirms that he has no conflict of interest.
ACKNOWLEDGEMENT
Declared None.


