All published articles of this journal are available on ScienceDirect.
Salvaging Left Testicular Fracture After a Motorcycle Accident: A Case Report
Abstract
Testicular fracture is a urological emergency that requires early diagnosis and timely surgical exploration in order to maximize testicular salvage. We presented a case of 17 year old male with left testicular fracture after roadside accident. The patient was surgically explorated and repaired with salvage of the injured testicle.
1. INTRODUCTION
Scrotal trauma accounts for less than 1% of all traumas that is attributed to the scrotum anatomy and mobility. Most of the scrotal traumas occur between ages 10 to 40 years [1]. Of these, blunt trauma is most prevalent form which primarily occurred due to motor vehicle collision, sport injury or assault [2]. Majority of these traumas occur in right testis due to its greater propensity to be trapped against the pubis or the inner thigh as compared to left testis [1]. Testicular rupture, sometimes referred as fractured testis, is a rare complication of testicular trauma and characterized by rip or tears in the tunica albuginea leading to the extrusion of testicular contents. Early surgical exploration and repair of the ruptured capsule is primarily recommended in these cases [3, 4].
2. CASE PRESENTATION
A 17-year-old haemodynamically stable male was admitted to our department after an injury from motor vehicle accident. The patient was alert, conscious and had normal vital signs but the pain and swelling over his left scrotal area were chief complaints. Subsequent evaluation showed non-distended, non-tender and soft abdomen. Examination of his genitalia revealed bruises on left scrotum with swelling and tenderness on palpation. Although, the left testis had no palpability due to swelling and pain but the right testis was palpable and non-tender. There was a superficial laceration wound measuring about 3 cm over left scrotal region with no active bleeding.
Ultrasound revealed the loss of normal configuration. The outline of the left testis was grossly enlarged, lobulated and heterogeneously hyperechoic with reduced vascularity at the affected area (Fig. 1). Furthermore, normal epididymis was not identified. The scrotal wall was grossly thickened and heterogeneous while spermatic cord showed normal vasculature (Fig. 2). However, the right testis retained normal configuration.


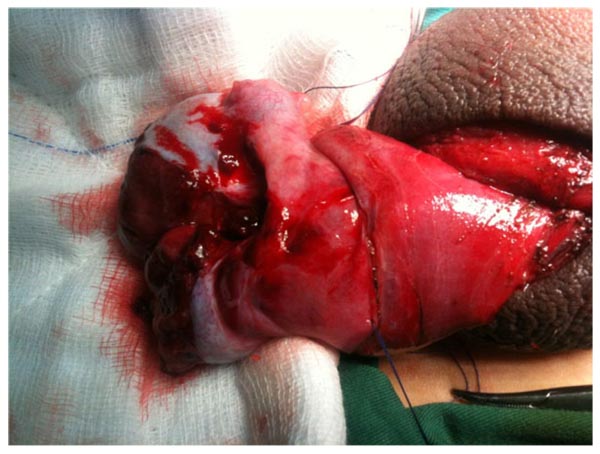
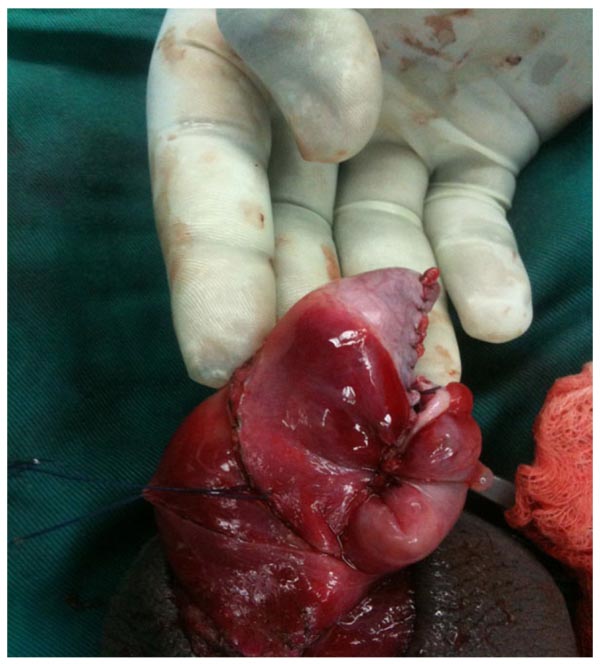
Scrotal exploration was carried out after taking consent from the parents. During exploration, both testicles were approached via a midline longitudinal incision. Hematoceles was evacuated by incision of the tunica vaginalis and both testes were delivered into the surgical field. Left testis was severely injured and transected in the middle (Fig. 3). Intratesticular hematomas were evacuated and the necrotic tubules and parenchyma was debrided. Vicryl 4-0 continuous suture was used to close tunica albuginea was closed with a 4-0 vicryl continuous suture (Fig. 4) and both testes were fixed posteriorly by using similar suture. A redivac drain was left and brought out through a stab incision into the scrotum.
Post-operative care consisted of antibiotic, analgesia and scrotal elevation. The patient had an uneventful recovery and was discharged on the third postoperative day. The patient was followed up in the urology clinic at post-discharge interval of 2 weeks, 1 month, 3 months, 6 months and one year. Patient was observed clinically well after one year of discharge and had no complain of pain. Doppler ultrasound of the testicles demonstrated normal and good blood flow to and within the both testes.
3. DISCUSSION
Traumatic testicle injuries may result from either blunt or penetrating trauma [5, 6]. Previously occurrence of blunt trauma to the external genitalia was rare; however, its incidence up to 50% has been documented in the literature [7]. Moreover, Bilateral testicular rupture has been documented in only five cases and its incidence is considered extremely rare [8]. Since size and location of the genitalia offers protection from the injury, it might be reason that testicular injury from penetrating trauma to the external genitalia rarely occurs [9]. Appropriate diagnosis of testicular rupture is of paramount importance. Patient`s history and physical examination should be served as mainstays during the management of testicular rupture. In condition where testicular salvage is necessary, surgical exploration should be immediately considered [10].
Exiting literature indicate the promising role of ultrasound along with physical examination as readily available noninvasive and highly accurate measures [1, 2]. However, there is a debate on the accuracy of ultrasound for testicular rupture due to its poor sensitivity [11] and misdiagnosis [12]. Nevertheless, more recent investigations reported acceptable sensitivity and specificity (95%) for diagnosing testicular rupture [1]. A great disparity in the management strategies of patients makes it difficult to evaluate the accuracy of ultrasound across published literature. In our institution all the patients with blunt scrotal trauma get benefits from the ultrasound. However, patients with abnormal clinical and ultrasound findings are managed surgically. In the current case, the results of scrotal ultrasound correspond to the intraoperative findings, reflecting the usefulness of ultrasound in the blunt scrotal trauma.
Conservative management for testicular rupture is accompanied by several complications that may lead to orchidectomy or testicular atrophy, therefore an early surgical exploration is advocated [1, 3]. Conservative approaches are recommended for patients with delayed presentation and include scrotal support, non-steroidal anti-inflammatory medications, ice packs, bed rest for 24–48 h and serial ultrasound [13, 14]. Nevertheless, exiting reports indicate the inverse proportional association of surgical delay and salvage rate, where delay in surgical interventions reduces the salvage rate from 80–90% to 45–55% and may necessitate orchiectomy [1, 15]. We operated our patient after 20 hours of trauma with successful testicular salvage. Most of the time, surgical interventions comprise of primary closure of the tunica albuginea and evacuation of the hematocele and debridement [1, 3, 15, 16]. In cases where viable extruded seminiferous tubules prevent closure of the testicular capsule, the wrapping of free edges of the tunica vaginalis around the extruded tubules followed by securing place with polyglactin can be peformed [3, 15, 16]. As compared to testicular torsion, where the arterial blood supply is completely compromised and requires immediate exploration, a testicular rupture is a relative ischemic state. Diagnostic delay in such instances may cause testicular ischemic necrosis, abscess and loss of spermatogenesis [16, 17]. Gangrenous infection is most dreaded intricacy of scrotal trauma, therefore pre and postoperative coverage of broad spectrum antibiotics should be encouraged. Testicular atrophy is a rare adverse outcome following rupture and might be attributed to ischemia and resorption due to increased pressure within the tunica secondary to hematoma formation. Fortunately, additional treatments are not required for this condition [1, 4]. Since recent investigations have revealed the superior diagnostic significance of computerized tomography imaging (CTi) as compared to ultrasonography (USG) for blunt intra-abdominal trauma [18, 19], we suggest more multicenter and large cohort studies to investigate the diagnostic utility of these techniques.
CONCLUSION
The incidence of testicular rupture is associated with either blunt or penetrating trauma. Quick assessment and diagnosis followed by scrotal exploration are mainstays in the management of acute testicular rupture. Growing body evidence proves legitimacy of timely surgical intervention where early interventions are accompanied by higher salvage rates and lowers risks of orchidectomy.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Current report was approved by the institutional review board to be published by not disclosing the identification of patients.
HUMAN AND ANIMAL RIGHTS
Animals did not participate in this research. All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2008.
CONSENT FOR PUBLICATION
An informed written consent was obtained from the patient to publish the study for research and academic purposes.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared None.


