All published articles of this journal are available on ScienceDirect.
Correlation of Warm and Cold Ischemic Time to Graft Function in Kidney Transplant: A Single Centre Report
Abstract
Background:
Kidney transplantation has been known as a major advancement of modern medicine which provides high-quality life years to patients with irreversible kidney failure (end-stage renal disease, ESRD) worldwide. The first kidney transplantation in Semarang was carried out at Telogorejo Hospital in 1985. Dr. Kariadi Hospital, has also undertaken kidney transplantation 28 times since January 2014 until September 2018. Kidney ischemic time is one of the most important factors which can affect the outcome of kidney transplantation. Prolonged ischemia of the graft can be related to transplantation’s effects. This study aimed to evaluate the influence of warm and cold ischemic time on the outcome of kidney transplantation in Dr. Kariadi Hospital Semarang.
Material and Methods:
This is an observational, cross-sectional study. The data was collected from medical record of all patients who underwent kidney transplantation from January 2014 until December 2018 and the level of creatinine and urine production before and after transplantation was documented. A total of 28 patients were registered and completed the inclusion criteria. The results of the study were tabulated and statistical analysis was performed using SPSS 23.0. The relationship was declared meaningful if p = 0.05 was obtained.
Result:
From the analysis of the research that has been done using the Pearson correlation test and hypothesis test Wilcoxon, it was found that there was a relationship between ischemic time and a decrease in creatinine level from r = -0.4489 with a value of p = 0.008. From the analysis of the research, a relationship between ischemic time and urine production was found after transplantation with a value of r = -0.562 and a value of p = 0.002.
Conclusion:
The results of this study show a strong correlation between the length of total ischemic time with a decrease in creatinine and urine production which means that the longer ischemic time, the lower the decrease in creatinine levels and the lesser the urine production.
1. INTRODUCTION
The number of patients diagnosed with End-Stage Renal Disease (ESRD) in Indonesia is increasing annually, showing similar trends with global prevalence [1, 2]. Kidney transplantation is acknowledged as a major advancement of modern medicine which provides high-quality life years to patients with ERSD worldwide [1, 3]. Patients who have kidney transplantation live 10 to 15 years longer than patients who undergo dialysis [4].
Since 1985, there have been several renal transplantations performed in Telogorejo Hospital and Dr. Kariadi General Hospital, Semarang. In Dr. Kariadi General Hospital Semarang, kidney transplantation have been done 26 times since January 2014 until September 2018 [5].
The success of kidney transplantation depends on several factors [6, 7]. Prolonged ischemia of the graft can be related to the effect of transplantation. Ischemia can induce a harmful cascade effect that can be worsened with the return of blood supply [8].This injury can produce an inflammatory and immune response that can potentially slow down the kidney function, increase alloimmune reactivation, and develop a progressive pathological change [9, 10].
The aim of this study was to investigate the influence of total ischemic time with the outcome of kidney transplantation in Dr. Kariadi General Hospital Semarang.
2. MATERIALS AND METHODS
This is an observational, cross-sectional study. The data was collected from the medical record of patients who underwent kidney transplantation from January 2014 until December 2018 at Kariadi General Hospital Semarang.
The population in this study are patients with renal failure who had kidney transplantation in Dr. Kariadi General Hospital Semarang. All the patients who underwent kidney transplantation having a medical record from January 2014 until December 2018 were examined for the level of creatinine and urine production before and after transplantation . There were 28 patients who were registered and completed the inclusion criteria.
Descriptive data is presented in the form of tables and box-plots. The normality test was conducted with Shapiro Wilk. Then the data was analyzed using the Wilcoxon test. The results of the study were tabulated and statistical analysis was performed using SPSS 23.0. The relationship is declared meaningful if p = 0.05 is obtained.
In clinical settings, patients with ESRD were actively screened as potential candidates for transplantation. Patients younger than 15 years old, older than 70 years, who were diagnosed with active systemic infection, active malignancy, significant cardiovascular, cerebrovascular or pulmonary disease, and drug/alcohol addiction were considered ineligible to become a recipient. Eligible and compliant patients with active National Health Insurance status were offered renal transplant program. The patient and family members were provided with the list of potential kidney donors. Potential donors who were willing to do the process were screened preliminarily before undergoing further tests to determine their suitability (Table 1).
| Variable | – | Recipient | Donor |
|---|---|---|---|
| Age | Mean (range) | 32.5 (15 – 50) | 46.8 (24 – 64) |
| Sex, n (%) | Male | 17 (63.0) | 14 (51.9) |
| Female | 10 (37.0) | 13 (48.1) |
Kidney transplantation and several renal transplantations are performed in Telogorejo Hospital and Dr. Kariadi General Hospital, Semarang. The number of transplants performed increases steadily every year (Table 2).
| Variable | N | % |
|---|---|---|
| Donor-recipient relationship | ||
| Related | 20 | 74.1 |
| Non-related | 7 | 25.9 |
| Etiology of ESRD | ||
| Hypertension | 16 | 59.3 |
| Diabetes mellitus | 4 | 14.8 |
| Autoimmune | 1 | 3.7 |
| Glomerulonephritis | 2 | 7.4 |
| Other | 4 | 14.8 |
| Recipient comorbidities | ||
| Coronary artery disease | 3 | 11.1 |
| Cerebrovascular disease | 3 | 11.1 |
| Pulmonary tuberculosis | 2 | 7.4 |
| Pleural effusion | 2 | 7.4 |
| Ascites | 2 | 7.4 |
| Hepatitis C | 2 | 7.4 |
| Gastric erosion | 1 | 3.7 |
| Depression | 1 | 3.7 |
| Recipients Body Mass Index | ||
| < 18.5 (underweight) | 4 | 14.8 |
| 18.5 – 24.9 (normal) | 14 | 51.9 |
| 25.0 – 29.9 (overweight) | 6 | 22.2 |
| ≥ 30.0 (obese) | 3 | 11.1 |
| HLA Matching | ||
| Full match | 20 | 74.1 |
| 4 miss match | 1 | 3.7 |
| 3 miss match | 1 | 3.7 |
| 2 miss match | 2 | 7.4 |
| 1 miss match | 2 | 7.4 |
The criteria for transplant recipients were the age of 15–70 years old, with at least one Human Leukocyte Antigen (HLA) matched with the donor and absence of Donor-Specific Antibody (DSA). Patients in Semarang showed similar demographics with the overall Indonesian cases, where most recipients were younger (33.0 years old) compared to the donors (46.1 years old) [11] Similarly, hypertension (61.5%) was the major etiology of ESRD. The recipient's comorbidities include cerebrovascular disease, coronary artery disease, history of pulmonary tuberculosis, pleural effusion, ascites, hepatitis C, gastric erosion and depression. The majority of the recipients received kidney from blood-related donors (n=19, 73.0%). There were 20 (76.9%) full HLA match, two cases of one and two miss match, one case of four and three miss-match. There were five (19.2%) cases of mortalities, two of them occurred during post-operative recovery period and the rest within 12 months after being discharged from the hospital. The cause of the two “early” mortalities was acute myocardial infarction (Table 3).
| Year | No. of Transplant | Mortality |
|---|---|---|
| 2012 | 1 | 0/1 |
| 2013 | 1 | 0/1 |
| 2014 | 3 | 2/3 |
| 2015 | 4 | 1/4 |
| 2016 | 4 | 2/4 |
| 2017 | 7 | 0/7 |
| 2018 | 7 | 2/4 |
The third death occurred 7 months post-transplant of a 39-year-old male with a history of myocardial infarction and gastric erosion. The cause of death was determined to be heart failure due to ischemic and hypertensive cardiomyopathy. Septic shock was the cause of death for the other two mortalities with one related to bacterial pneumonia and the other with unknown primary site of infection. There were three cases of allograft rejection, one patient with three pre-transplant HLA miss match and the other with two HLA miss-match. Post-transplant immunosuppressive regiment was discontinued and all three patients underwent dialysis again. This is the first report that presents the total number of kidney transplants performed in Indonesia. The number has risen significantly within the past 5 years, especially in medical centers in Java. However, it is still far below from what is needed or when compared to neighboring Southeast Asian countries like Vietnam, Thailand, and Philippines [12, 13] Several barriers to transplantation in Indonesia that had been previously elaborated include shortage of specialists, high cost, lack of easy access and information within the community, as well as amongst the medical practitioners.
The situation of kidney transplantation in Semarang was affected by the events elaborated by Mochtar et al. (Level Of Evidence 4). The first recorded kidney transplant in Semarang was in 1977. Afterwards, there were several unrecorded kidney transplants, mainly performed in Dr. Kariadi General Hospital. The renal transplant system was formally restarted in 2014 and since then, the procedure has been regularly performed in the institution. In–hospital ESRD patients are individually offered the transplant program by the nephrologist team. Although there has been a constant annual increase of kidney transplant performed since 2014, the manual patient recruitment system will eventually limit the center from ever reaching its maximum potential.
The average waiting time for patients in Semarang was 68 months from the start of enrollment until the operation. The waiting time and the total number of transplants can be greatly increased by a coordinated National database online system. We report on 27 cases of living- donor transplantations from January 2012 until July 2018. In contrast, Cipto Mangunkusumo Hospital in Jakarta performed 491 transplants within 6 years. There were five (19.2%) mortalities in Semarang, all within 12 months post-transplant. The mortality rate is similar to Jakarta (n=28, 20.28%) as reported by Marbun et al. In Semarang, two patients (40.0%) died during post-operative recovery due to acute myocardial infraction, one patient (20.0%) died because of cardiomyopathy, and two patients (40.0%) by sepsis. The main cause of death in Jakarta was sepsis (n=8, 40.0%), followed by an unknown cause (n=7, 35.0%), pulmonary edema (n=2, 10.0%), hepatitis (n=2, 10.0%) and stroke (n=1, 5.0%). Marcelino et al. published the only Indonesian data available for comparison, which was based on Laparoscopic Living-Donor Nephrectomy (LLDN) technique. In terms of procedural time, the average first Warm Ischemic Time (WIT) of open technique in Semarang was longer compared to the LLDN in Jakarta (6.6 minutes vs. 4.3 minutes). Expectedly, the average intraoperative blood loss was also higher in open technique (384 ± 192 mL vs. 194 ± 198 mL). However, no urinary retention, operative wound site infection or severe pain (Visual Analogue Scale ≥7) was recorded (Table 4).
| Procedural Time | Minutes: Seconds |
|---|---|
| Warm ischemic time I | 06: 34 |
| Cold ischemic time | 08: 04 |
| Warm ischemic time II | 27: 55 |
| Total ischemic time | 36: 56 |
Based on the outcome of 17 patients that surpassed the 12–month mark, the 1–year survival rate of a transplant patient in Semarang is 70.6%. Compared to Jakarta, the 1- year survival is 88.5% and 3-year survival is 79.7% [11]. Compared to abroad, the 1-year survival rates for living donor kidney transplants are 97.2% in the United States, 98.0% in Australia and New Zealand, 95.8% in Europe, and 97.7% in Canada. The limited number of transplants in Semarang contributes to the low survival rates. It also highlights the need for training and expertise. Better survival rate can be achieved with more transplants number as well as reaching the plateau of learning curve within the coming years. The transplant team in Semarang is also in the process of applying LLDN technique to achieve better operative results (Table 5).
| Intraoperative bleeding, mean (SD) in mL | 384 (±192) |
| Hospital stay, mean (range) in days | 11 (10 – 14) | |
| Infection, n (%) | 2 | (7.7) |
| Cardiovascular, n (%) | 3 | (11.5) |
| Total number of deaths, n (%) | 5 | (19.2) |
| Re-dialysis, n (%) | 3 | (11.5) |
| Re-transplant, n (%) | 0 | (0.0) |
Based on this study, there was an improvement in the total number of kidney transplantations between January 2012 to July 2018 at Dr. Kariadi Hospital Semarang. The main cause of ESRD is hypertension. Most recipients are younger than the donor with majority kidney sources being blood-related donor.This report shows that 1-year survival rate in Semarang is lower than others center. Exclusive hospital-patient communication and medical record system for kidney transplant patients is also being established to ensure a long-term and complete follow–up. The initial goal of our institution is to establish a firm kidney transplant center capable of covering Central Java, aiding the decentralization of kidney transplantation in Indonesia that can be considered to be still in its infancy. There has been a consistent increase in kidney transplantation, however still concentrated within the capital city. Major barriers that have been surmounted include the establishment of National Health Insurance full coverage in 11 appointed hospitals and a National law that permits organ transplantation. As of 2018, the five leading centers that performed the most transplants are Jakarta, Surabaya, Yogyakarta, Semarang and Malang. Currently, there are limited Indonesian data to compare the intra and post-operative results of our center. However, improved experience and expertise are imperative to achieve better and satisfactory results in Semarang. At national level, continuous efforts are being made for the expansion of specialists’ training programs and kidney transplantation centers. There is an ongoing yet intangible effort by the Indonesian National Transplantation Society in establishing an organ procurement system for a cadaveric donor, public education, and the ever-needed Transplant National Database.
3. RESULTS
3.1. Creatinine Level
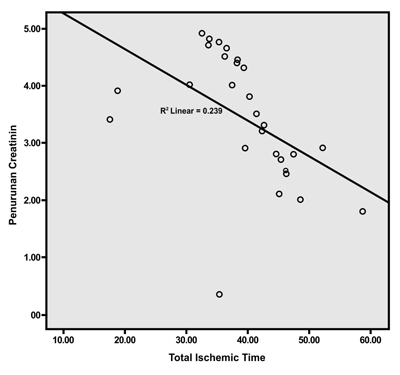
The results of the research conducted on 28 study subjects found that before and after transplantation as many as 28 subjects had decreased creatinine (Fig. 1). From the analysis carried out, we obtained creatinine average before the transplant to be 7.9 ± 2.53, mean creatinine value after surgery 5.2 ± 4.4, and mean creatinine decrease 3.4 ± 1.1 mg/dL. From the analysis of the research using Pearson correlation test and hypothesis test Wilcoxon, it was found that there was a relationship between ischemic time and a decrease in renal postin creatinine from r = -0.4489 with a value of p = 0.008 (Fig. 2).
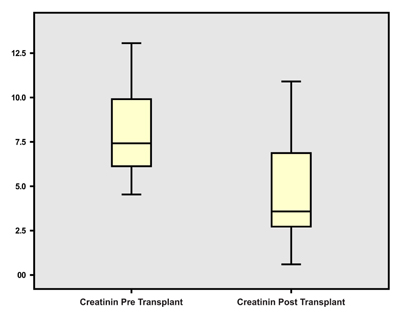
3.2. Urine Production
The results of the study conducted on 28 research subjects found that the average urine production 2.5 hours post anastomosis was 294 ± 87 ml. From the analysis of the research, there is a relationship between Ischemic Time and post-transplant urine production with a value of r = -0.562 and a value of p = 0.002 (Fig. 3).
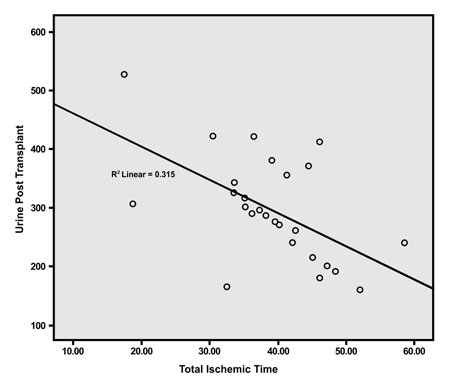
4. DISCUSSION
Chronic Kidney Disease (CKD) is damage to the structure or function of the kidney lasting ≥ 3 months, with or without a decrease in Glomerular Filtration Rate (GFR) [11]. The successful kidney transplantation depends on some factors such as ischemic time. [6, 7] Total ischemic time is defined as the time of the donor renal artery interruption or aortic clamp, until the time of release of the clamp on the renal artery in the recipient (in hours). Total ischemic time is a combination of Cold Ischemic Time (CIT) and Warm Ischemic Time (WIT). [12, 13] Prolonged ischemic time is associated with an increase of Delayed Graft Function (DGF) and longer length of stay which consequently increase the cost of transplantation [14, 15].
Reperfusion after CIT activates the complex cascade, which ultimately contributes to apoptotic or necrosis cell death. This phenomenon is also known as Ischemic Reperfusion Injury (IRI) [8]. It is known that injuries caused by ischemia and reperfusion and to some extent also with cooling and rewarming give rise to cascades which ultimately lead to apoptosis, endothelial cell injury, and activation of the innate immune response resulting from organ dysfunction [10].
DGF occurred in 13.5% of recipients with a total ischemic time of 14 hours or longer than 10.9% of those with shorter ischemic time. This effect is greater for those with donors aged 55 years or more. Thus, it appears that the consequences of a long ischemic time are mainly identifiable in the early posttransplant period as DGF and possibly an increased acute rejection rate. The effects of ischemic time on the long-term outcome of renal transplantation in the form of impaired graft function and graft survival are less evident [10, 16].
CONCLUSION
From the results of this study, there is a strong correlation between the length of total ischemic time with a decrease in creatinine levels and urine production which means that the longer ischemic time, the lower the decrease in creatinine levels and consequently the lesser the urine production.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Written informed consent was obtained from all the participants.
AVAILABILITY OF DATA AND MATERIALS
- The article used to support the findings of this study have been deposited in the Ethnicity & Disease, Volume 16, Spring 2006. https://www.google.com/url? sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=2ahUKEwi4xafokLPiAhU363MBHQO_BZ0QFjAAegQIBhAC&url=https%3A%2F%2Fwww.ethndis.org%2Fpriorsuparchives%2Fethn-16-2s2-14.pdf&usg=AOvVaw3PK9yA_gCjqIB8hj8469Qt
- The article used to support the findings of this study have been deposited in PLoS One. 2016 Jul 6;11(7):e0158765. doi: 10.1371/journal.pone.0158765.
- The article used to support the findings of this study have been deposited in https://www.google.com/url? sa=t&rct=j&q=&esrc=s&source=web&cd=2&cad=rja&uact=8&ved=2ahUKEwi2uJe2k7PiAhXS7XMBHUncCnEQFjABegQIBBAB&url=https%3A%2F%2Fwww.pernefri.org%2F&usg=AOvVaw183-YUJkiaDeQigB9G0Yhm
- The article used to support the findings of this study have been deposited in https://www.google.com/url? sa=t&rct=j&q=&esrc=s&source=web&cd=1&ved=2ahUKEwisoc7ok7PiAhVh7nMBHeN_DrQQFjAAegQIBBAC&url=http%3A%2F%2Fwww.european-renal-best-practice.org%2Fsites%2Fdefault%2Ffiles%2FBoekje%2520niertransplantatie%2520Indonesian%2520OKDRUK.pdf&usg=AOvVaw0FU86CQLlyk_5F9H-Bs0sy
- The article used to support the findings of this study have been deposited in Asian Jurnal of Urology avalilable online 22 February 2019.
doi: https://doi.org/10.1016/j.ajur.2019.02.003. - The article used to support the findings of study have been deposited in Transplant Proc. 2010 Jun;42(5):1413-20.
doi: 10.1016/j.transproceed.2010.04.016. - The article used to support the findings of study have been deposited in Am J Transplant. 2013 May;13(5):1134-48.
doi: 10.1111/ajt.12210. Epub 2013 Apr 8. - The article used to support the findings of study have been deposited in Kidney Int. 2015 Feb;87(2):343-9.
doi: 10.1038/ki.2014.304. Epub 2014 Sep 17. - The article used to support the findings of study have been deposited in Kidney Int. 2015 Feb;87(2):272-5.
doi: 10.1038/ki.2014.359. - The article used to support the findings of study have been deposited in Am J Kidney Dis. 2002 Feb;39(2 Suppl 1):S1-266
- The articel used to support the findings of study have been deposited in Transplantation. 2017 Jun;101(6): 1152-1158.
doi: 10.1097/TP.0000000000001351. - The article used to support the findings of study have been deposited in Transplant Direct. 2018 May; 4(5): e342. Published online 2018 Apr 18.
doi: 10.1097/TXD.0000000000000781. - The article used to support the findings of study have been deposited in Transplantation. 2019 Feb;103(2): 401-411.
doi: 10.1097/TP.0000000000002309. - The article used to support the findings of study have been deposited in Transplant Direct. 2017 Jul; 3(7): e177. Published online 2017 Jun 23.
doi:10.1097/TXD.0000000000000680. - The article used to support the findings of study have been depoited in Curr Opin Organ Transplant. 2013 Apr;18(2):174-8.
doi: 10.1097/MOT.0b013e32835e2a08.
FUNDING
Not applicable.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
The author would like to thank the editorial board and all staff of Renal Transplant Team Dr. Kariadi General Hospital Semarang, for their support to this research.


