All published articles of this journal are available on ScienceDirect.
A Complicated “Simple” Renal Cyst
Abstract
Background:
Simple renal cysts are usually asymptomatic and benign. Rarely, symptoms and complications can develop from local mass effect which is illustrated by this case.
Case Presentation:
77 year old Caucasian male presents with abdominal pain for five days. Abdominal exam was diffusely tender, markedly distended, tympanic with absent bowel sounds. His work-up included an abdominal x-ray showing a colonic obstruction and abdominal CT showing a large 27 cm renal cyst. Drainage of the renal cyst resolved obstructive symptoms.
Conclusion:
A simple renal cyst should not be overlooked as the reason for acute abdominal pain. Simple renal cysts, though benign are not without complications.
INTRODUCTION
Simple renal cysts are usually found incidentally with the increasing use of abdominal diagnostic ultrasonography (U/S) or computed tomography (CT) for other causes. A distinct characteristic is their increased occurrence with aging. Autopsy studies report almost half of people older than 50 years of age have one or more renal cysts. They are usually unilateral, solitary and asymptomatic. We report a case in which a simple cyst deviated from its common set of features [1-4].
CASE PRESENTATION
This case is a 77 year old Caucasian male with a history of chronic abdominal pain due to a 15 cm renal cyst (last measured 7 years ago) and stage 4 chronic kidney disease with a recent AV fistula placed in preparation for dialysis who presents with diffuse abdominal pain for five days. The abdominal pain gradually worsened and was diffuse in location but worse in the lower quadrants. The pain was aggravated by eating and there were no alleviating factors. The patient reported a non-productive cough, shortness of breath at rest and exertion (at baseline), poor appetite, abdominal distention over the past week, diarrhea and no bowel movements for the past two days, dysuria, lower extremity swelling, easy bruising, and dizziness. The patient denied vision changes, fevers, chills, muscle aches, chest pain, palpitations, nausea, vomiting, melena, hematochezia,
tenesmus, flatus, hematuria, and change in urinary frequency, weakness and skin changes.
On admission, the patient was afebrile with blood pressure of 146/70 mmHg, heart rate of 122/minute and irregularly irregular, respiratory rate of 16/minute, and oxygen saturation of 93% on 4 liters nasal cannula. Though the patient was in no acute distress and lying comfortably in bed, examination revealed a diffusely tender abdomen that was markedly distended and tympanitic to percussion without bowel sounds.
Laboratory findings are listed in Table 1. Admission imaging included a chest x-ray and abdominal x-ray (Table 2). Subsequently, a nasogastric tube and rectal tube were inserted. The physical exam remained unchanged with these interventions. A CT of the abdomen and pelvis without contrast (Figs. 2-5) was performed (Table 2). It was believed that the large renal cyst was causing a colonic obstruction. To further characterize the cyst and determine its true origin a renal ultrasound (U/S) and magnetic resonance imaging (MRI) of the abdomen were done (Table 2).
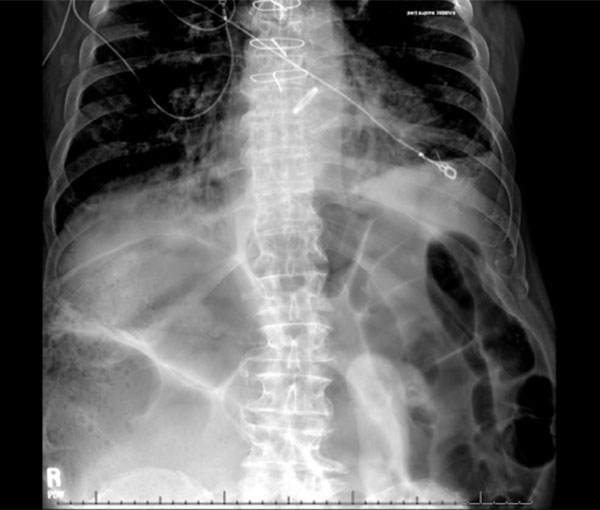
Abdominal x-ray demonstrating dilated colon due to a possible distal colonic obstruction.
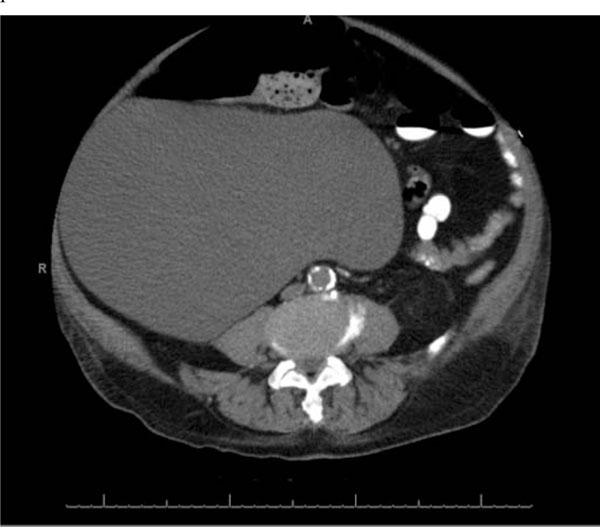
CT of Abdomen/Pelvis demonstrating 27 cm renal cyst.
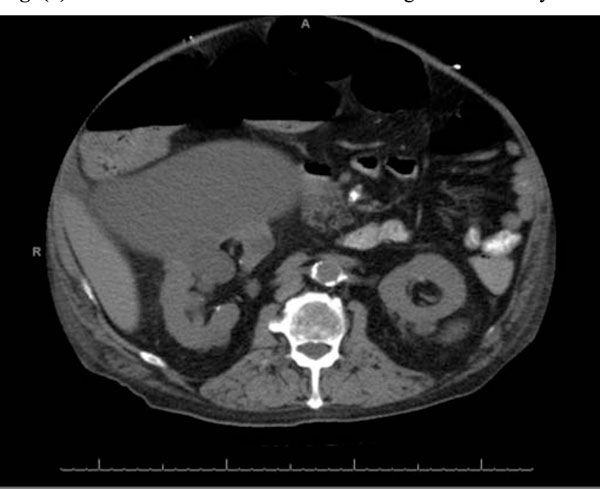
CT of the Abdomen/Pelvis demonstating the renal cyst originating from the right kidney.
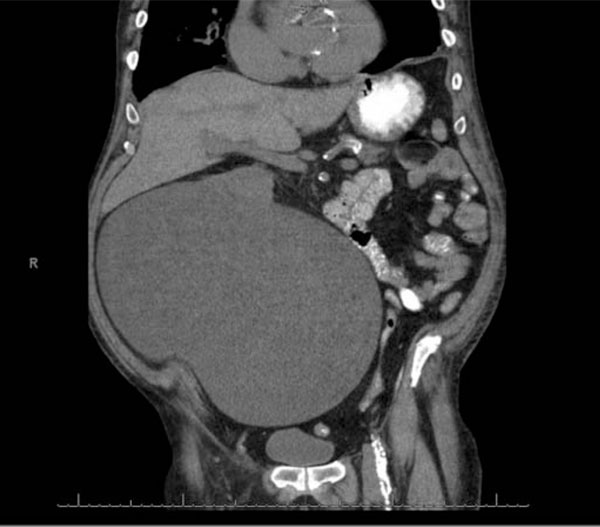
CT of the Abdomen/Pelvis (coronal view) demonstrating a large renal cyst.
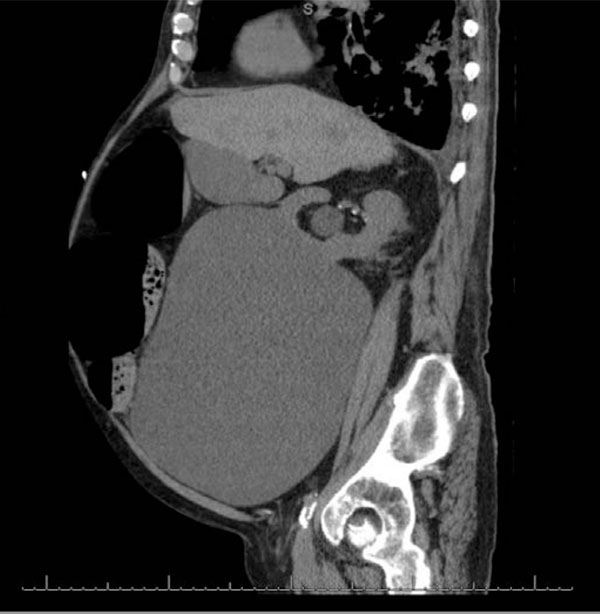
CT of the Abdomen/Pelvis (sagittal view) deomonstrating a large renal cyst.
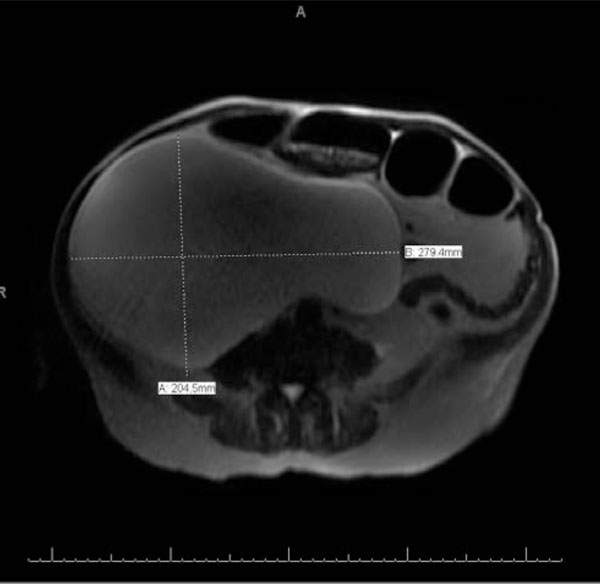
MRI of the Abdomen demonstrating a right renal cyst measuring 27.94 cm by 20.45 cm.
Laboratory Values
| Laboratory | Value | Normal Value |
|---|---|---|
| White Blood Cell | 18 k/uL | 4.5-11 k/uL |
| Hemoglobin | 10.8 g/dL | 13-18 g/dL |
| Hematocrit | 32.8% | 40-52% |
| Platelets | 234 k/uL | 150-440 k/uL |
| Sodium | 140 mEq/L | 135-145 mEq/L |
| Potassium | 5.3 mEq/L | 3.5-5 mEq/L |
| Chloride | 107 mEq/L | 99-19 mEq/L |
| Bicarbonate | 28 mEq/L | 22-33 mEq/L |
| BUN | 49 mg/dL | 6-20 mg/dL |
| Creatinine | 1.95 mg/dL | 0.6-1.2 mg/dL |
| Glucose | 76 mg/dL | 70-105 mg/dL |
| Calcium | 9 mg/dL | 8.5-10.5 mg/dL |
| Phosphorus | 3 mg/dL | 2.9-4.8 mg/dL |
| Magnesium | 2.4 mg/dL | 1.6-2.6 mg/dL |
| AST | 36 U/L | 10-37 U/L |
| ALT | 35 U/L | 10-49 U/L |
| Alkaline Phosphatase | 48 U/L | 41-120 U/L |
| Total bilirubin | 0.9 mg/dL | 0.3-1.2 mg/dL |
| Total protein | 5.6 g/dL | 6.2-8.3 g/dL |
| Albumin | 3.3 g/dL | 3.4-4.9 g/dL |
| Brain natriuretic peptide | 404 pg/mL | < 100 pg/mL |
| Troponin | 0.25 ng/mL | < 0.1 ng/mL |
| CKMb | 3.6 ng/mL | < 10 ng/mL |
| CPK | 37 U/L | 32-294 U/L |
| Lactic acid | 1 mmol/L | 0.5-2.2 mmol/L |
| INR | 2.8 | 2.5-3.5 Aortic Valve Replacement |
| PT | 26.9 seconds | 9.7-11.3 seconds |
| aPTT | 25.8 seconds | 23-31 seconds |
| Urine analysis | Cloudy, Yellow, specific gravity 1.015, pH 5, 1+ proteins, negative glucose, negative ketones, negative bilirubin, 20-50/HPF RBCs, 2+ hemoglobin, 5-19/HPF WBC, 1+ leukocyte esterase, negative nitrites, normal urobilinogen, few epithelial cells, granular casts | Clear, Yellow, specific gravity 1.005-1.030, pH 4.5-8, negative proteins, negative glucose, negative ketones, negative bilirubin, 0/HPF RBCs, negative hemoglobin, 0/HPF WBC, negative leukocyte esterase, negative nitrites, normal urobilinogen |
Imaging Studies
| Imaging Study | Finding |
|---|---|
| Electrocardiogram | Atrial fibrillation with a heart rate of 110/minute, T wave inversions in the lateral leads which was unchanged from prior ECG |
| Chest x-ray | Enlarged cardiac silhouette, bilateral interstitial edema, blunting of the left costophrenic angle consistent with pleural thickening or pleural effusion. |
| Abdominal x-ray (Fig. 1) | Multiple moderately dilated, gas filled loops of colon noted in the upper abdomen suggesting a possible distal colonic obstruction. |
| Renal ultrasound | Renal cysts without evidence of obstructive uropathy, a very large cystic mass in the right mid-abdomen possibly due to a very large exophytic right renal cyst versus a peritoneal inclusion cyst or cystic retroperitoneal neoplasm or intraperitoneal neoplasm. |
| CT abdomen and pelvis without contrast (Figs. 2-5) | Bilateral pleural effusions, coronary calcifications, bladder distention, a large cystic mass that is believed to be renal in origin measuring 27 cm possibly originating from the right kidney |
| MRI abdomen without contrast (Fig. 6) | Multiple renal lesions some of which appear to represent cysts though they cannot be completely characterized without contrast, very large cystic lesion in the right abdomen of indeterminate significance, tiny pancreas fluid signal intensity lesions, evidence of iron deposition in the liver and spleen, T2 bright lesions in the liver possibly reflective of hemangiomas or cysts though not completely characterized, and cardiomegaly |
Bosniak Renal Cyst Classification. Adopted from Eknoyan G. A Clinical View of Simple and Complex Renal Cysts. J Am Soc Nephrol 20: 1874-1876, 2009
| Category | Cyst Wall | Septae | Calcification | Enhancement |
|---|---|---|---|---|
| I | Hairline thin | No | No | No |
| II | Minimal regular thickening | Few, hairline thin | Smooth, hairline thin | No |
| IIF | Minimal regular thickening | Multiple, minimal smooth thickening | Thick, nodular | No |
| III | Irregular thickening | Measurably thick, irregular | Thick, nodular, irregular | Yes |
| IV | Gross irregular thickening | Irregular gross thickening | Thick, nodular, irregular | Yes, tissue and cyst |
Due to the ongoing abdominal pain, distention, lack of bowel movement/flatus and worsening lactic acidosis (to 3.8 mmol/L), an U/S guided drainage of the renal cyst was performed; 6.7 liters of serous fluid were drained. A catheter was placed for continuous drainage which produced about 0.5 liters in the following two days and was subsequently removed. The fluid cultures were negative for growth.
After the drainage, the patient had improvement of his abdominal pain and distention. He began to produce flatus and small bowel movements.
DISCUSSION
Renal cysts are a common finding in the general population especially with the increasing use of CT and ultrasound. Renal cysts increase in frequency after the second decade of life. The prevalence can range from 5-41% depending on the imaging modality used to diagnose renal cysts [1, 2]. About 20% of 40 year old patients and 33% of those older than 60 years old have renal cysts. Common risk factors for renal cysts include advanced age, male gender, renal dysfunction, hypertension, and the need for long-term dialysis [2, 4].
Early hypotheses suggested that renal infarction and tubular obstruction was the inciting events that lead to the development of a renal cyst. Recent theories focus on the diverticula of the distal convoluted tubules as the etiology of cysts. A renal tubule detaches from its parent tubule thus creating a potential space. These diverticula increase in number in the aged kidney, probably as a result of weakening of the tubular basement membrane [1, 2, 4, 6, 7].
Renal cyst classification is based on their appearance and enhancement on CT and was introduced by Bosniak in 1986 with the most recent revision in 2003 [1,11,12]. The
Bosniak classification (Table 3) is based on the fluid density, wall and septal thickness, enhancement, and calcification which helps classify chances of being benign versus malignant. It was developed for CT but can be applied to MRI or U/S [8-2].
This patient had Bosniak category I (simple) renal cysts. The cyst was a discrete lesion within the kidney likely of cortical origin extending beyond the parenchyma and distorting the renal contour [1]. This category of cysts is oval to round with a smooth border of single layer of flattened cuboidal epithelial cell. These cysts are filled with a homogeneous transudate-like, clear or straw-colored fluid of low viscosity, with a radiodensity similar to water [1, 7]. Approximately 70 to 80% are solitary, unilateral, and cortical [1].
Risk factors that predispose one to rapid and aggressive cyst enlargement include younger age at time of diagnosis, renal cyst being multiloculated, and bilateral renal cysts [4]. Simple renal cysts vary in size, but enlarge over time in approximately 25% of cases at a rate of 3.9% per year. They may double in size over 10 yr [1, 2]. A younger age at the time of measurement is the strongest predictor [4].
Most simple renal cysts are asymptomatic and incidentally discovered, requiring no intervention. Infrequently, simple renal cysts can cause mass effect as a complication that requires intervention, as in this case [9]. A large renal cyst may cause obstructive symptoms, particularly when proximal to or encompassing the renal pelvis [1]. Most renal cysts are placed superficially and expand away from the kidney and can, on occasions, reach sufficient size to press on neighboring structures, such as the stomach or colon, to produce dyspepsia and obstruction. For example, the only case report found was from 1914 involving an extremely large renal cysts, containing as much as 12 liters of fluid [6]. The symptoms of these large renal cysts are due to pressure on surrounding organs including chronic intestinal obstruction as described in 1914 by Bevers et al. [5]. In this 1914 case report, the region of the colon at the splenic flexure was constricted where it passed around the neck of the renal cyst and the cyst itself was pressing upon the descending colon causing a second obstruction [5]. Complications are rare with a range of 2 to 4% [1]. The most common complications are hemorrhage, infection, or rupture. Hemorrhage may occur in a preexisting simple renal cyst, or a renal cyst may form from the liquefaction of a traumatic hemorrhage within the kidney parenchyma, which occurs in about 6% of simple renal cysts. Simple renal cysts may become infected or a renal abscess may resolve into a renal cyst. The wall of infected renal cysts is often thickened markedly and calcified occasionally. Attenuation is increased and may be nonhomogeneous but is not enhanced after dye [1].
The management of renal cysts is largely dependent upon its Bosniak score. Bosniak category I and II cysts are benign, but may need periodic evaluation by U/S for the first 2 to 3 years, especially in younger patients with cyst diameters greater than 3 cm [1]. The decision for intervention in Bosniak category I or II cysts largely depends upon the effects and symptoms directly related to renal cyst. If an intervention is decided, the options include: percutaneous management, aspiration, sclerotherapy, surgical de-roofing, open surgery, laparoscopic surgery, standard multiple-port access surgery, single-port laparoscopic surgery, and robot-assisted surgery [2, 7, 9]. One study showed that continuous percutaneous catheter drainage with negative pressure was more efficient than single-session alcohol sclerotherapy in large renal cysts [10]. Laparoscopic renal cyst ablation can also be offered to patients who have symptomatic simple renal cysts and who have failed previous conservative management and a trial of sclerosing agents or percutaneous aspiration [2]. Follow-up is recommended for Bosniak category IIF lesions. The time interval required to diagnose a renal mass as benign is not known. Bosniak category III and IV patients are referred for consideration of surgical removal due to high malignancy rates [8].
CONCLUSION
Colonic obstruction due to a simple renal cyst is unusual with only one case report in 1914. The idea is not completely out of the ordinary especially if the renal cyst is large enough. Recognizing which renal cyst need follow-up is also a key component. Even though simple renal cyst usually do not need follow-up, large renal cysts should be followed. Once symptoms arise, it is up to the primary care physician to recognize the complications and symptoms related to renal cyst. If this patient had followed up with a renal U/S, it would have been recognized earlier and interventions could have prevented the colonic obstruction. Also in the elderly, these types of complications need to be recognized sooner so as to avoid deleterious outcomes such as death.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.


